Friday 14 May is National ODP Day, when the nation is invited to celebrate one of its lesser-known allied health professions, the operating department practitioner.
Anyone who’s had a surgical procedure of some kind will be familiar with the ODP, without knowing it. An ODP is the person who prepares you for anaesthetic and reassures you in that nervous period before a procedure. There will also be an ODP in the recovery room, ensuring all is well as you return from surgery, and making those initial moments when you regain consciousness far less strange than they might be.
At the same time, there’s another person we never see – the “scrub ODP”, who works with the surgical team during the procedure, and whose role includes preparing the surgical instruments and handing the correct instrument at the right time to the surgeon.
In other words, ODPs play a major role in every stage of a person’s operation – anaesthetic, surgery and recovery. Individuals are trained to diploma or degree level to perform all of these roles, though often focus on one.
These unsung but highly skilled health professionals really are worth celebrating. And many ODPs are UNISON members.
The theme of this year’s National ODP Day is ‘Celebrating personal and professional diversity’, the aim to encourage ODPs everywhere to share their stories of how they came to the profession and the highlights and challenges of the job.
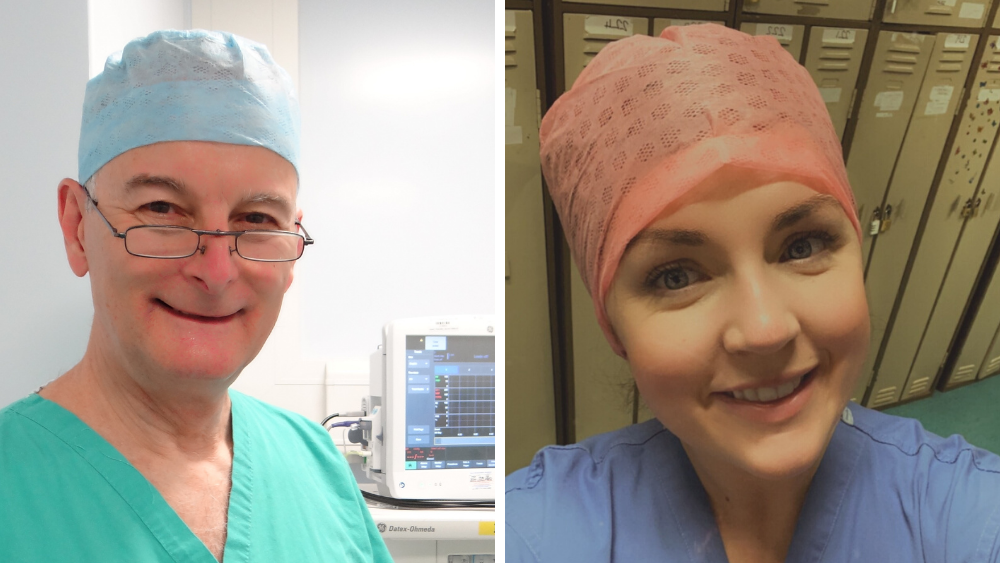
Simon Broughton, 67, has been an ODP for some 40 years. Having trained and begun his career at Lowestoft Hospital in Suffolk, he’s since worked for a number of London’s specialist and teaching hospitals, and is currently based in Hertfordshire. He’s worked as a locum, through agencies, for more than half his career.
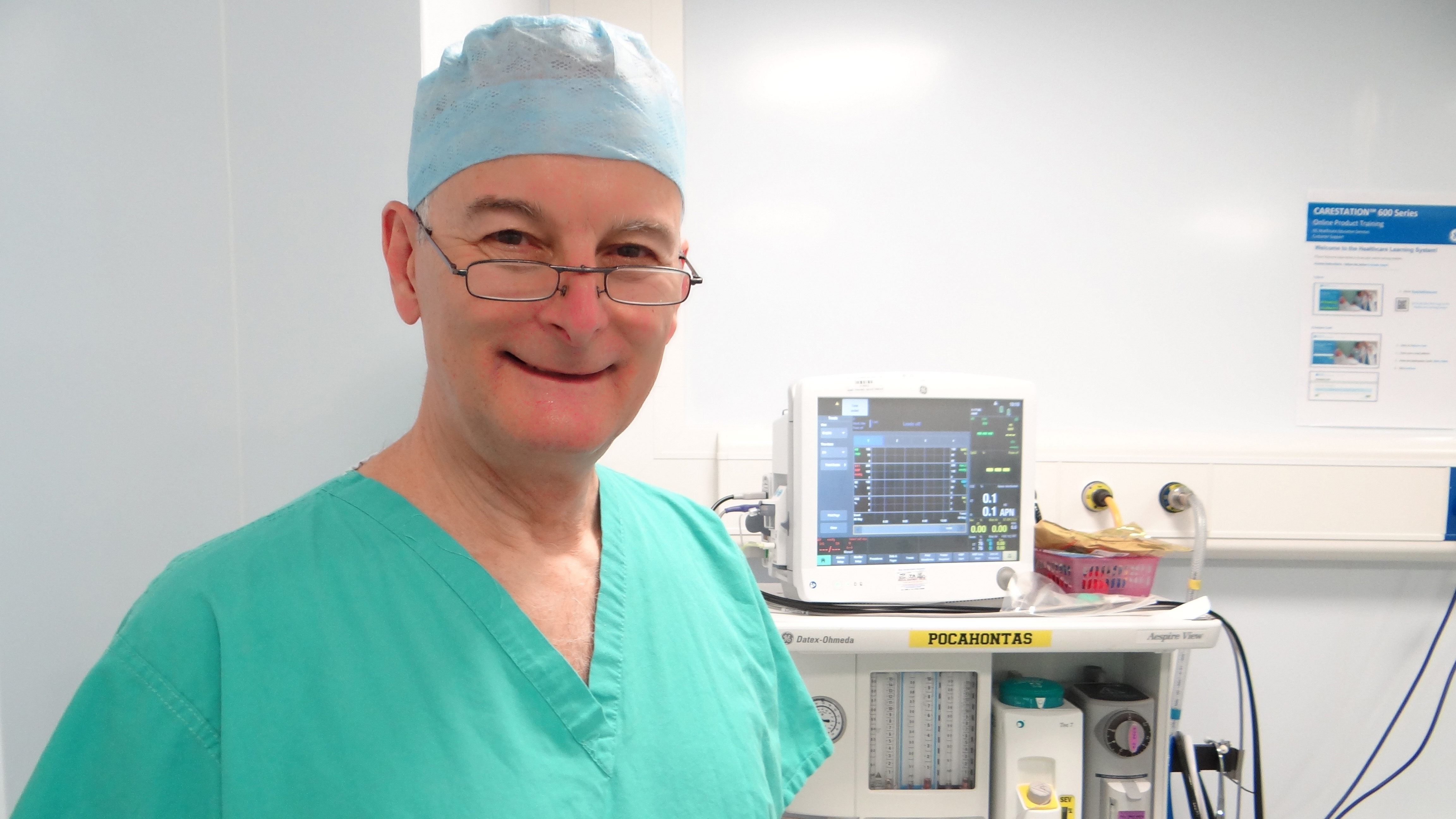
“I specialise in anaesthetics, so I’m with the patient from when they arrive in the anaesthetic room until they leave theatre for recovery, where I hand the patient to the recovery team.
“You may have a consultant anaesthetist and a junior anaesthetist involved, or just one of them, plus the ODP. I have to check the patient’s ID and ask them relevant questions, for example if they’ve been starved – because one of the hazards of anaesthesia is the aspiration of stomach contents, which can be a killer.
“A very important aspect of our task is to reassure the patient and inspire confidence, to create an atmosphere of calm assurance in which they can go to sleep easily.
“I used to specialise in paediatric cardiac anaesthesia – anaesthetising tiny babies with heart defects. This is obviously a frightening thing. You have the parents in the anaesthetic room with you, in pieces, knowing these could be their last moments with their child alive. I find the best way to ensure a smooth process is to talk to the patient – even if it’s the tiniest baby. And with babies I found that I was also speaking for the benefit of the parents, so they would be informed of what was going to happen and feel they’re doing the best for their child.
“The smallest patient I’ve ever had was a premature baby of only 400grams, who I held in one hand. At the other end of the scale, I had a patient who then was the tallest man in the world, according to the Guinness Book of Records. I can’t remember how tall, but I had to borrow another operating table from another theatre, and put the two end-to-end, so we could have a table long enough!
The unsung heroes of the operating room – and now the pandemic
“When I first started we didn’t have the inventions we have now, like O2 and CO2 monitors. The first sign that a patient was depleted of oxygen was when they turned blue! We had to watch them like a hawk. Since then there have been so many fantastic inventions and improvements in technique and this job is a never-ending learning process.
“And as a locum I’ve worked in lots of different hospitals, with all sorts of different anaesthetists, which for me was a great learning experience. So I’ve been able to use my experience in more recent years in helping other members of staff do things more easily.
“I’ve kept in good shape all my life. And the older I get the more I seem to enjoy the job. It can a very difficult and stressful job at times, but very rewarding as well.
“Work during the pandemic has been a bit erratic, because of the cancellation of almost all elective work. So that has impacted on me in the last year and a bit. But it’s about to pick up. I think we’re all going to be very, very busy in the next couple of years.”
Laura Smith, 36, is a second year ODP trainee in Glasgow, studying for her diploma. She previously worked as a dental nurse for 13 years, but was keen for a career change and became a healthcare support worker, working in hospital theatres. After two years in that role, and having fallen in love with the theatre environment, she jumped on the chance to become an ODP.

“I’m loving my training and have enjoyed every placement I’ve experienced so far. I’ve met some amazing people and have learned so many new skills. The first case I actually watched was a hip replacement. Straight away I thought, ‘I just love this.’
“Luckily I’m not squeamish at all. I find it fascinating. I think it’s amazing the things surgeons can do, and how everyone works together as a team. Theatres are very much about the teamwork.
“Placements are hands-on, but with mentors always there. It’s certainly a challenge, trying to learn all the different specialities. You can learn to scrub for an orthopaedic case one day, and then for a plastic surgery case the next, and they’re completely different instruments, completely different skills, completely different operations.
“The maternity placement has been a complete eye-opener for me. Anaesthetics in maternity feels very, very different, because the patient’s awake. For a caesarean section we give them a spinal anaesthetic, so they’re numb from the chest down, but they’re still completely aware of everything that’s going on. So you’re trying to assure them that they’re going to be OK.
“When I qualify I want to work in Glasgow Royal Infirmary, where you can do scrub and anaesthetics without having to choose between them, which is absolutely ideal. I want to do both.
“I recently made a wee, 60-second TikTok video about my journey so far and it’s had over 36,000 views and prompted so many questions about the profession, along with words of encouragement from total strangers. I do wish more people knew exactly what an ODP can do and what our skill set is, so it’s amazing if I’ve just raised a teeny bit of awareness.”







♡♡♡♡♡♡♡♡♡♡…NAM MYOHO RENGE KYO NAM MYOHO RENGE KYO…♡♡♡♡♡♡♡♡♡♡♡♡♡♡…I REALLY LIKE BOTH ARTICLES…AND THEY ARE QUIET UNINSPIRING!!!
THANK YOU VERY FOR YOUR GOOD WORK!!!THANK
♡♡♡♡♡♡♡♡…NAM MYOHO RENGE KYO NAM MYOHO RENGE KYO…♡♡♡♡♡♡♡…xxxXxxx…♡♡♡♡♡♡♡♡